-
Healthcare Delivery
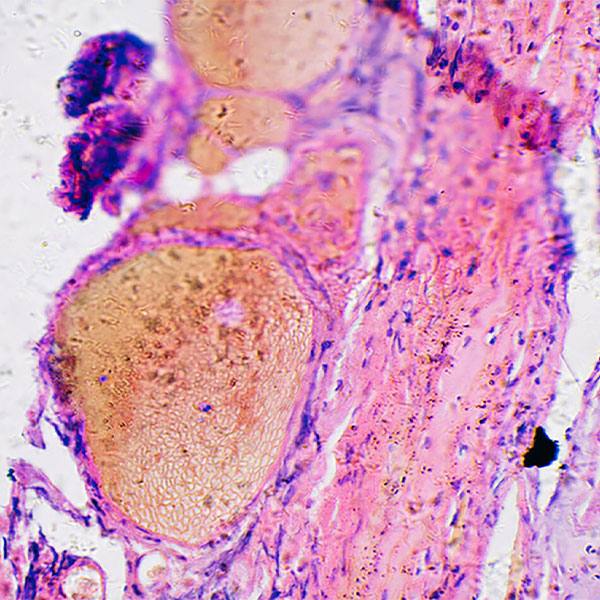
Candida auris: This fungus is a health care concern
Fungi live just about everywhere, including on and inside of the body. Fungal infections are more common in people with weakened immune systems, or when fungi are introduced to areas where they are not normally found, such as in a wound.
Candida species are the most common yeast responsible for fungal infections. Many fungal infections are not life-threatening and can be easily treated with antifungal medicines. But a specific type of Candida called Candida auris is on the rise and can cause serious and often fatal infections.
Candida auris was first discovered in Japan in 2009. It has spread to dozens of countries around the world, including the United States. This fungus is dangerous and is a concern in health care facilities because the infection spreads easily, resists drug therapy and is difficult to treat. More than 1 in 3 patients with an invasive Candida auris infection die, according to the Centers for Disease Control and Prevention (CDC).
Where is Candida auris?
Candida auris often presents as a bloodstream infection or a wound infection, or even an ear infection. It can also be found in urine or respiratory specimens but its significance there is unclear. An infected person may have a fever and chills that don’t improve after a normal course of antibiotic therapy.

Candida auris can be spread from one patient to another, often through contaminated surfaces and equipment. It can survive in the environment for a long time and withstand some commonly used disinfectants.
Between 2020 and 2021, Candida auris cases in U.S. health care facilities rapidly increased, and they continue to be on the rise. The CDC now considers the fungus an urgent antimicrobial resistance threat. In addition, the World Health Organization (WHO) has placed Candida auris in the critical priority group on its fungal priority pathogens list.
“Its characteristics are not distinct enough to allow scientists to tell it apart from the other species by just looking at it under a microscope,” says Nancy Wengenack, Ph.D., a clinical microbiologist at Mayo Clinic.
“Specialized laboratory tests such as a targeted PCR (polymerase chain reaction) assay or culture followed by MALDI-TOF (matrix-assisted laser desorption/ionization-time of flight) mass spectrometry are needed to definitively identify Candida auris. A lack of proper testing and diagnosis could lead to delayed or inappropriate treatment.”
Who is at risk of infection?
Patients in health care facilities who are immunocompromised or already critically sick from other illnesses are most at risk for Candida auris infection. Patients with IV lines or other invasive medical devices are also at risk as these can be potential entryways for the fungus to enter the bloodstream.
“The average healthy person should not panic,” says Dr. Wengenack. “But the CDC has alerted U.S. health care facilities to watch out for this infection in patients so that special precautions can be taken to prevent and control its spread.”
How is it diagnosed and treated?
Candida auris colonization can be detected through a laboratory screening test performed using a swab of the patient's underarm and groin area. Infection can be detected using standard fungal cultures of blood and other specimens.
Close consultation with an infectious disease specialist is required to determine the best course of treatment for an infected person.
“This infection is often treated with the echinocandin class of antifungals. But, there has been a recent rise in echinocandin-resistant strains, which is concerning,” says Dr. Wengenack. “Combination antifungal therapy and some of the new investigational antifungals have been used for those echinocandin-resistant strains.”
What infection prevention methods can be used?
This fungal species survives longer than other Candida species in the environment for reasons that are not well understood yet. Health care facilities should be vigilant in surveillance screening so the proper precautions can be used to protect patients, health care workers and visitors.
Using proper hand hygiene is critical to preventing the spread of all microbes and infections including Candida auris. It is also important to use cleaning agents that are active against Candida auris, such as bleach.
“A lot of research is still needed in this area,” says Dr. Wengenack. “Hospitals and health care providers are partnering with the WHO, the CDC, and public health officials to learn how best to detect, contain and prevent the spread of Candida auris."
"The good news is clinical laboratories have robust methods available to detect and accurately identify Candida auris," she says. "This should help in the efforts to contain the spread of this emerging global pathogen.”
—Luci Gens
Editor's note: This article was updated on June 9, 2023 with a clarification on how Candida auris is transmitted.
Related Articles