-
Cancer
A Powerhouse of Cancer Research: A View from Florida
Nearly everyone has been affected by cancer, either through a personal diagnosis or that of a loved one. In the U.S., 1.7 million people are diagnosed each year, and over 15 million survivors are alive today, according to the National Cancer Institute.
Mayo Clinic takes a distinctive all-hands-on-deck approach to this deadly disease. Clinicians and researchers work side by side, developing groundbreaking therapies to provide patients with answers, treatment options and optimism.
The Mayo Clinic Cancer Center, which spans Mayo Clinic's Arizona, Florida and Minnesota locations, has 10 distinct research programs funded by the National Cancer Institute that are centered on broad areas such as immunology and gene therapy, or specific tumor types such as brain and gastrointestinal. Each research topic is treated with a multidisciplinary approach that ties together science, clinical relevance and prevention — a depth and breadth that lends itself to discovery and patient application.
Mayo Clinic Cancer Center enjoys the National Cancer Institute's prestigious comprehensive cancer center designation, which recognizes scientific leadership, resources and research. It also demonstrates an organization's willingness and ability to work rigorously across disciplines to solve complex issues and propel new and better treatments.
"The bar is high. This acclaim is a badge of honor," says Tushar Patel, M.B., Ch.B., dean for research at Mayo Clinic in Florida. "It indicates that we've achieved excellence in patient care and research that advances cures."

Innovative research projects are underway at all three Mayo Clinic Cancer Center locations in Arizona, Florida and Minnesota. Read on for an overview of research projects at Mayo Clinic in Florida that are driving breakthroughs for the benefit of patients at Mayo and beyond.
Vaccines and viruses: Recruiting the immune system
In one approach, scientists within Mayo Clinic Cancer Center's Cancer Immunology and Immunotherapy Program are finding new ways to support a patient's immune system to help the body compete with cancer. "Recruiting the immune system to fight disease has become so important to cancer research," says Roxana Dronca, M.D., a Mayo Clinic oncologist and hematologist.
Dr. Dronca and her colleagues are working to find biomarkers that could help providers understand which patients are most likely to respond to immunotherapy.

"These expensive treatments carry a risk of side effects. We want to know from the outset if they're likely to have an effect," says Dr. Dronca.
For this, she works closely with Haidong Dong, M.D., Ph.D., a Mayo Clinic molecular immunologist.
"Identifying biomarkers can be a fishing expedition," Dr. Dronca says. "Instead, our mechanistic approach has led us to what we think are fairly robust biomarkers."
Dr. Dronca's team also is involved in testing whether oncolytic viruses — viruses that infect tumors but not normal cells — can serve as a therapy for metastatic melanoma, a type of advanced skin cancer that is frequently deadly.
"Mayo has developed a number of these exciting viral therapies for patients who have exhausted other treatment options," she says.
Another immunotherapy leader at Mayo Clinic in Florida, Keith Knutson, Ph.D., is on the brink of making a once far-fetched idea — a vaccine for cancer — a reality. "Our team is finding remarkable results," he says. "We're not just excited. We're ecstatic."
Dr. Knutson and colleagues, including Matthew Block, M.D., Ph.D., a Mayo Clinic immunologist, are focused on developing vaccines that boost the immune system to prevent the recurrence of breast and ovarian tumors in patients who've undergone traditional cancer treatment. Early data show that their ovarian cancer vaccine may be able to reduce the recurrence rate of this disease to 60%, down from nearly 90%.

"What more can we do for patients, safely, after they've been treated for cancer? We are finding ways to support their immune system so they can continue to fight these tumors," says Dr. Knutson.
And while current research is focused on patients at high risk for cancer or its recurrence, Dr. Knutson's team already is looking ahead with the hope of someday preventing cancer on a population level, like vaccines for measles or the flu.
Chimeric antigen receptor therapy (CAR-T cell therapy): A game changer for lymphoma and more
Another promising new area of cancer research and treatment is CAR-T cell therapy, an individualized treatment that uses a patient's own cells to fight cancer. Mayo Clinic was the first cancer center in Northeast Florida to offer CAR-T cell therapy.
"CAR-T cell therapy has improved the prognosis for patients with large B cell lymphoma, a common blood cancer in adults," says Mohamed Kharfan Dabaja, M.D., a Mayo Clinic bone marrow transplant and lymphoma expert, of this leading-edge technology. "Whereas before, less than 20% of patients would survive 18 months, with CAR-T therapy, more than 50% can survive this aggressive disease."
Dr. Kharfan Dabaja and colleagues also are studying the potential for CAR-T cell therapy to help patients with chronic lymphocytic leukemia and, soon, acute myeloid leukemia.
His team also is investigating new ways to optimize blood and marrow transplantation, in which healthy blood stem cells are used to treat cancer.
"These are complex procedures that require immense logistical and technical capabilities, as well as a multidisciplinary approach — major strengths to which Mayo patients have access," Dr. Kharfan Dabaja says.
Researching the delivery of custom treatments
At the other side of the research continuum, investigators within Mayo Clinic Cancer Center's Cell Biology Program are transforming scientists' understanding of cancer by studying how it is created, and how it grows and spreads.
For example, a team led by Panagiotis Anastasiadis, Ph.D., a Mayo Clinic cancer cell biologist, has discovered that adhesion molecules, which help cells arrange properly in a tissue, suppress tumor growth by regulating small RNAs, which are called micro-RNAs.

"Adhesion molecules are so commonly misregulated in cancer that a better understanding of their interplay with micro-RNAs may lead to novel treatments with wide applicability to breast, lung, pancreatic and other cancers," he explains.
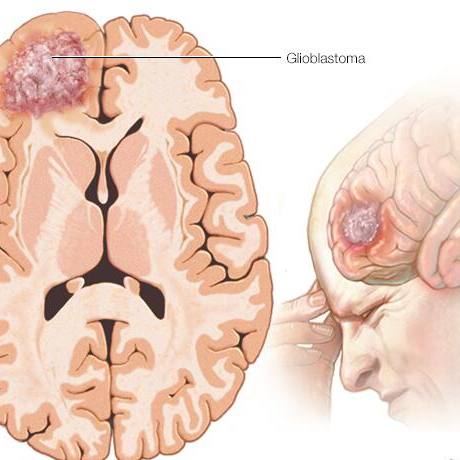
Dr. Anastasiadis and his colleagues also are attempting to increase survival rates for patients with glioblastoma, an aggressive form of brain cancer.
"In 30 years of glioblastoma research, we've seen basically no appreciable increase in survival," he says.
His team is studying proteins and pathways that are essential for the aggressive growth and the dissemination of glioblastoma cells into normal brain cells. If these can be identified, they may be optimal targets for new therapies. "We believe we're making progress on something that could significantly improve survival," he says.
Finally, because Dr. Anastasiadis believes that one of the most important new approaches to cancer is personalized treatment, he and colleagues across Mayo Clinic in Arizona, Florida and Minnesota are collaborating with Mayo Clinic's Center for Individualized Medicine to develop and test a new strategy to improve cancer care. In this initiative, scientists take a sample from a patient's tumor, subject it to a number of high-tech analyses, and convene a multidisciplinary team to identify which existing therapies are most likely to work in each case. Then their suggestions are tested in the laboratory using miniature 3D cultures of the patient's original tumor. If a cancer treatment is found to be effective there, then it could be used to help the individual.
"Not only is this a testament to what's possible for individualized medicine, it's a way for cancer researchers to work closely with clinicians to help patients," says Dr. Anastasiadis.
The entire spectrum of care
The research of Dr. Patel's team is focused on liver cancer, the second leading cause of cancer death worldwide. The scientists are harnessing the potential for particles secreted by cells — called extracellular vesicles and extracellular RNA — to lead to earlier diagnosis and improved therapy. Their work is backed by the National Institutes of Health's Common Fund, which supports high-risk but potentially transformative concepts.
The field of liver cancer is an example of the breadth of care available to patients that sets Mayo Clinic apart.
"We're one of very few centers across the nation where patients have access to the entire spectrum of treatment — from surgery, transplant, radiation and chemo to early-phase clinical trials," Dr. Patel says. "A liver cancer patient at Mayo will have an expert available in every capacity. They'll have every option available."
The National Cancer Institute recognized Mayo's expertise in liver cancer and bile duct cancer in 2018 by awarding the Mayo Clinic Cancer Center the nation's first Hepatobiliary SPORE grant.
Research that puts patients first
This level of care is continuously elevated by Mayo's patient-centric cancer research, Dr. Patel says.
"Mayo Clinic Cancer Center's designation as an NCI comprehensive cancer center means patients can feel confident about the standards of excellence being met in the lab, which lead to excellence in their care," says Dr. Anastasiadis. "That's the goal of all this research — to affect care. That's the special element we provide to Mayo patients."
Mayo Clinic researchers also note the importance of the National Cancer Institute designation for building partnerships with other cancer centers.
"You're always stronger if you're part of an integrated team," Dr. Dronca says.
These partnerships take place outside of as well as within Mayo. Mayo Clinic Cancer Center is the only comprehensive cancer center with three geographic sites.
"We're very much symbiotic with Mayo Clinic in Arizona and Minnesota, each with particular areas of strength to share," Dr. Dronca says.
In addition, Mayo's continual technology and infrastructure investments add to the high caliber of research and its reputation for translating discoveries into new treatments for cancer patients at Mayo Clinic in Florida.
Above all, Mayo Clinic cancer scientists expressed gratitude to their patients for donating the blood and tissue samples that make this research possible.
"The people we care for are central to helping us discover new treatments," says Dr. Dronca. "Patients want to help us to turn their experience into something that can help someone else. We are so fortunate that patients are willing to help us learn for the greater good."
Sara Nick, December 2019