-
Aging
Mayo Clinic Research News – Zombie Cell Edition
There are times when a cell must cease its work. In an embryo, it’s when a hand must separate into fingers. In wound healing, it’s when further scar tissue formation would do further harm rather than helping. It could come at the end of a normal cell’s limited number of divisions, or when a cell is heading down a pathway that leads to cancer.
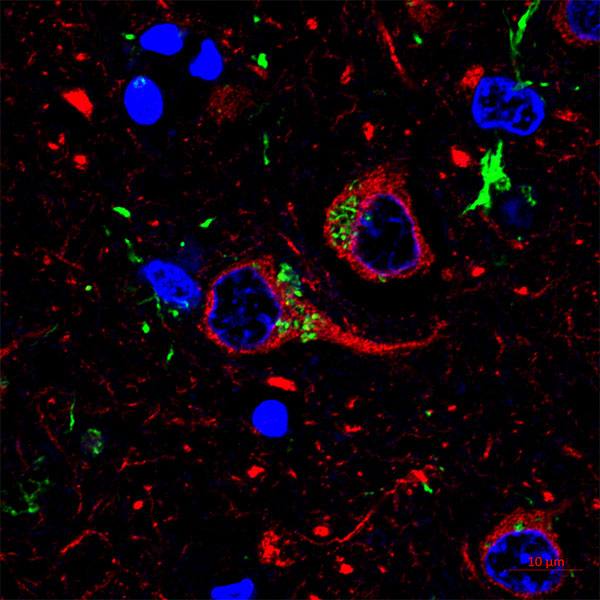
Cells that are stopped from dividing but that refuse the body’s order to die, and instead exude an array of protein signals that change the tissue around them, are called senescent cells. These cells, sometimes called zombie cells, are implicated in conditions of aging, ranging from osteoporosis to diabetes and muscle weakness.
Mayo Clinic researchers are in the forefront of these investigations into how senescent cells contribute to these illnesses and what might be done to treat them. Here are some recent findings on senescent cells, from Mayo scientists and collaborators.

Credit: Donna DeSmet, Mayo Clinic medical illustration/animation
Faulty Mitochondria Trigger Senescent Cell Signals
The array of signals sent out by senescent cells changes the environment around the cell for both good and ill. It can call in immune cells to a site where damaged cells must be removed, but it can also result in chronic inflammation. Taken as a whole, these signals are called the senescence-associated secretory phenotype. Since these signals have both positive/negative results, an international group of researchers began looking at how the signals are regulated to provide a framework for modulating them: keeping the good, ditching the bad.
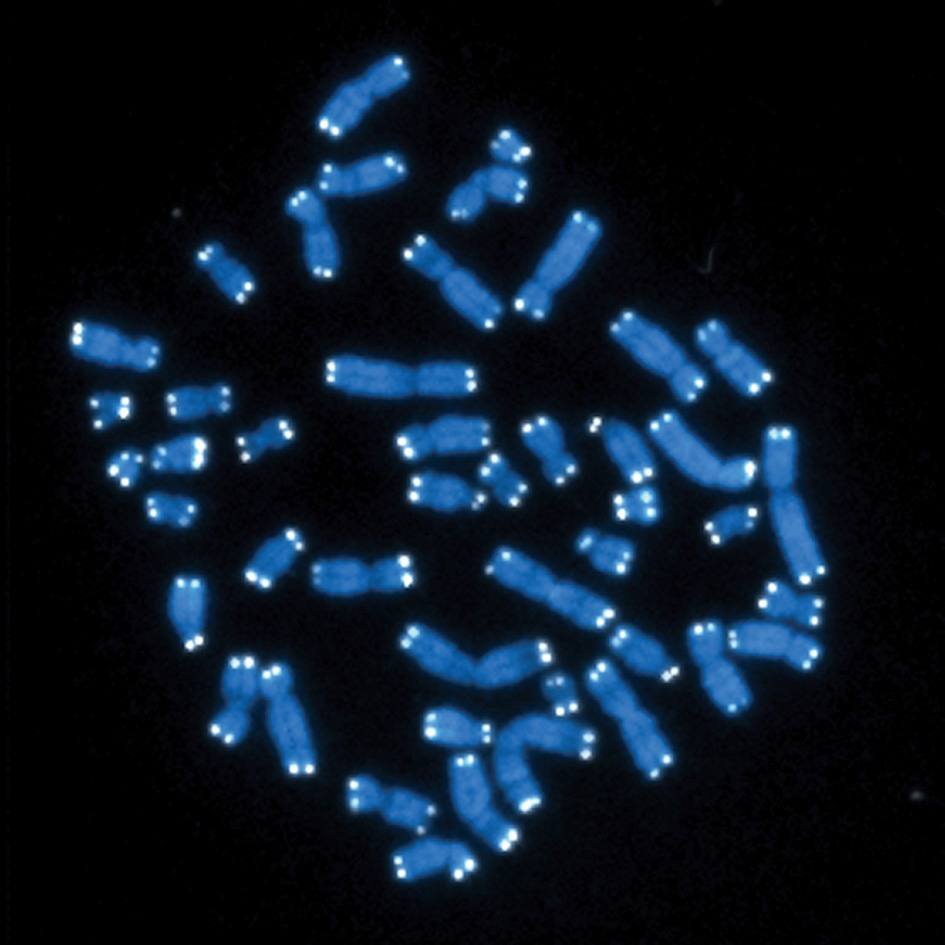
The team, including authors from the University of Glasgow, Harvard University and Harvard Medical School, Massachusetts General Hospital, Sanford Burnham Prebys Medical Discovery Institute, Newcastle University and Mayo Clinic, report that signals from dysfunctional mitochondria to the nucleus result in bits of chromatin — a complex of proteins, DNA and RNA in the nucleus — fragmenting into pieces and pushing into the cell’s cytoplasm.
Published in the journal Genes and Development, the authors write that detection by the cell of random the chromatin fragment triggers the inflammatory senescence-associated secretory phenotype. The authors also report that this action presents a biological target for future drug development. This research was supported, in part, by Ted Nash Foundation. Mayo Clinic authors include Anthony Lagnado, Ph.D., João Passos, Ph.D., Patrick J. Kruger and Diana Jurk, Ph.D.
Obesity linked to Senescence of Mesenchymal Stem Cells in Cell Culture
In the journal Frontiers in Cell and Developmental Biology, Mayo researchers report that obesity increases senescence and diminishes the function of fat-tissue derived mesenchymal stem cells in comparison to the same type of cells from non-obese controls. These adult stem cells are present throughout the body and can renew tired or damaged tissue. The researchers report on samples from 40 subjects who donated fat tissue.
The findings suggest that obesity may limit the vigor and ability of these stem cells to do their work, contributing to the tissue damage and organ injury linked to obesity. They also write that obesity induces cellular senescence, senescence-associated secretory phenotype and inability to divide in mesenchymal stem calls, linked to severity of obesity. This research was supported by the National Institutes of Health, the Burroughs Wellcome Fund, the Connor Fund, Rob and Terry Ryan Foundation, and Noaber Foundation. Authors, all from Mayo Clinic, include Sabena Conley, Ph.D., and senior author Lilach Lerman, M.D., Ph.D., the Arthur M. and Gladys D. Gray Professor in Honor of Dr. Howard A. Andersen.
Senescent Cells, Chemotherapy and Bone Loss
In a mouse model, researchers from Washington University School of Medicine and Mayo Clinic found that senescent cells contribute to chemotherapy-induced bone loss. The authors of the paper published in the journal Cancer Research report that this finding is independent of mouse estrogen levels, and so suggests a new mechanism of bone loss during treatment that could be explored. They further found that when senescent cells were depleted, bone density was preserved in the mice treated with chemotherapy. This research was supported, in part, by the Glenn Foundation for Medical Research and National Institutes of Health funding. Mayo Clinic authors include Darren Baker, Ph.D.